Feldene
By J. Thorek. University of South Carolina, Aiken. 2019.
Mode of transmission—Ingestion of the organisms in under- cooked meat purchase feldene 20mg with amex, contaminated food and water purchase 20mg feldene, or raw milk; from contact with infected pets (especially puppies and kittens), farm animals or infected infants. Contamination of milk usually occurs from intestinal carrier cattle; people and food can be contaminated from poultry, especially from common cutting boards. Incubation period—Usually 2 to 5 days, with a range of 1–10 days, depending on dose ingested. Period of communicability—Throughout the course of infection; usually several days to several weeks. The temporary carrier state is probably of little epidemiological importance, except for infants and others who are incontinent of stool. Chronic infection of poultry and other animals constitutes the primary source of infection. Susceptibility—Immune mechanisms are not well understood, but lasting immunity to serologically related strains follows infection. In developing countries, most people develop immunity in the first 2 years of life. Preventive measures: 1) Control and prevention measures at all stages of the food- chain, from agricultural production on the farm to process- ing, manufacturing and preparation of foods in both commer- cial establishments and the domestic environment. Use irradiated foods or thoroughly cook all animal foodstuffs, particularly poultry. Avoid common cutting boards and re- contamination from uncooked foods within the kitchen after cooking is completed. Comprehensive control programs and hygienic measures (change of boots and clothes; thorough cleaning and disinfection) to prevent spread of organisms in poultry and animal farms. Good slaughtering and handling practices will reduce contamination of carcases and meat products. Puppies and kittens with diarrhea are possible sources of infection; erythromycin may be used to treat their infections, reducing risk of transmission to children. Control of patient, contacts and the immediate environment: 1) Report to local health authority: Obligatory case report in several countries, Class 2 (see Reporting). Ex- clude symptomatic individuals from food handling or care of people in hospitals, custodial institutions and day care cen- tres; exclude asymptomatic convalescent stool-positive indi- viduals only for those with questionable handwashing habits. In communities with an adequate sewage dis- posal system, feces can be discharged directly into sewers without preliminary disinfection. Identification—A mycosis usually confined to the superficial layers of skin or mucous membranes, presenting clinically as oral thrush, intertrigo, vulvovaginitis, paronychia or onychomycosis. The single most valuable laboratory test is microscopic demonstration of pseudohyphae and/or yeast cells in infected tissue or body fluids. Culture confirmation is important, but isolation from sputum, bronchial washings, stool, urine, mucosal surfaces, skin or wounds is not proof of a causal relationship to the disease. Candida (Torulopsis) glabrata is distinguished from other causes of candidiasis by lack of pseudohyphae formation in tissue. Mode of transmission—Contact with secretions or excretions of mouth, skin, vagina and feces, from patients or carriers; by passage from mother to neonate during childbirth; and by endogenous spread. Susceptibility—The frequent isolation of Candida species from sputum, throat, feces and urine in the absence of clinical evidence of infection suggests a low level of pathogenicity or widespread immu- nity. Oral thrush is a common, usually benign condition during the first few weeks of life. Local factors contributing to superficial candidiasis include interdigital intertrigo and paronychia on hands with excessive water exposure (e. Uri- nary tract candidiasis usually arises as a complication of prolonged catheterization of the bladder or renal pelvis. Most adults and older children have a delayed dermal hypersensitivity to the fungus and possess humoral antibodies. Preventive measures: Early detection and local treatment of any infection in the mouth, oesophagus or urinary bladder of those with predisposing systemic factors (see Susceptibility) to prevent systemic spread. Fluconazole chemoprophylaxis de- creases the incidence of deep candidiasis during the first 2 months following allogenic bone marrow transplantation. Anti- fungal agents that are absorbed fully (fluconazole, ketocon- azole, itraconazole) or partially (miconazole, clotrimazole) from the gastrointestinal tract have been found to be effective in preventing oral candidiasis in cancer patients receiving chemotherapy. Control of patient, contacts and the immediate environment: 1) Report to local health authority: Official report not ordinarily justifiable, Class 5 (see Reporting). Topical nystatin or an azole (miconazole, clotrimazole, ketoconazole, flucon- azole) is useful in many forms of superficial candidiasis. Oral clotrimazole troches or nystatin suspension are effec- tive for treatment of oral thrush. Itraconazole suspension or fluconazole is effective in oral and oesophageal candi- diasis. Epidemic measures: Outbreaks are most frequently due to contaminated intravenous solutions and thrush in nurseries for newborns. Identification—First described in Luzon, Philippines, in the early 1960s, the disease is clinically an enteropathy with massive protein loss and a malabsorption syndrome leading to progressive weight loss and emaciation.
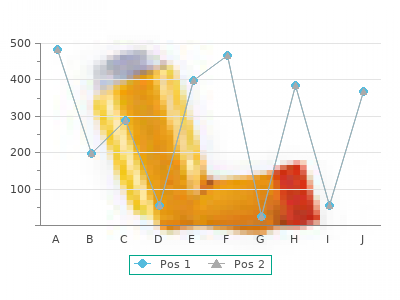
About one-third of children (for example generic feldene 20 mg fast delivery, measles) buy feldene 20mg otc, or it may be prolonged, as under 2 years of age experience an episode of in persons with the acquired immunodeficiency rotavirus diarrhoea. When immunosuppression is person to person and possibly also through severe, diarrhoea can be caused by unusual respiratory secretions as well as faeces. Some strains produce Diarrhoea can result from viral, bacterial or parasitic only one type of toxin, some both. Today, using new techniques, experienced laboratories can Shigella Page 59 identify pathogens in about 75% of cases seen at a Shigella is the most common cause of dysentery, treatment facility and up to 50% of milder cases present in about 60% of all episodes, and in nearly detected in the community. Tissue Mixed infections involving two or more destruction and possibly watery diarrhoea are enteropathogens occur in 5–20% of cases seen at caused in part by the extremely potent Shiga toxin, health facilities. Diarrhoea may be severe, leading to with their faeces or consumption of contaminated dehydration and collapse within a few hours if the food, milk, or water. In endemic diarrhoea (two-thirds of cases) or dysentery (one third areas cholera occurs mostly in children, adults have of cases). Cryptosporidium This is a coccidian parasite that causes disease in Salmonella infants, immunodeficient patients and a variety of Most Salmonella infections can be traced to domestic animals. In developing countries infection infected animals or contaminated animal products. Thereafter, infections are usually most developing countries, but may be important asymptomatic. Diarrhoea is usually neither severe in communities where commercially processed nor prolonged, except in immunodeficient patients, foods are widely used. Antibiotics are not In such individuals, Cryptosporidium is an effective, and may cause delayed clearance of important cause of persistent diarrhoea with Salmonellae from the intestinal tract. A number of other pathogens can cause diarrhoea in young children although their importance is not Others pathogens that may be of local importance well defined. They include: include: • Viruses: Norwalk agent, enteric adenoviruses • Vibrio cholerae 01 in endemic areas and • Bacteria: Aeromonas hydrophila, enteroadherent during epidemics; Escherichia coli, enteroinvasive Escherichia coli, Page 60 Module 3 enterohaemorrhagic Escherichia coli, Plesiomonas during the warm season, whereas viral diarrhoeas, shigelloides, Vibrio cholerae non-O group 1, particularly disease caused by rotavirus, peak during Vibrio parahaemolyticus, Yersinia enterocolitica the winter. In tropical areas, rotavirus diarrhoea • Protozoa: Giardia lamblia, Entamoeba tends to occur throughout the year, increasing in histolytica, Isospora belli. The incidence of persistent diarrhoea of healthy children under 3 years of age, making it follows the same seasonal pattern as that of acute difficult to know whether a pathogen isolated watery diarrhoea. This is especially true for Giardia lamblia, Most enteric infections are asymptomatic, cysts of which are found nearly as often in healthy especially in those over 2 years of age owing to the children as in those with diarrhoea; it is also true development of active immunity. On the other hand, which time stools contain infectious viruses, Shigella and rotavirus are rarely identified in healthy bacteria, or protozoal cysts. Persons with children; their presence in a child with diarrhoea asymptomatic infections play an important role in strongly indicates that they are the cause of the the spread of many enteric pathogens, especially illness. Intermediate areas include the southern European countries (eastern and western) and the Now carry out Learning Activity 2. Manifestations There are three types of diarrhoea: Page 61 Distinct seasonal patterns of diarrhoea occur in • acute watery diarrhoea; many geographical areas. In temperate climates, • dysentery; and bacterial diarrhoeas tend to occur more frequently • persistent diarrhoea. Module 3 Page 61 Acute watery diarrhoea • There is no single microbial cause for persistent • Starts acutely diarrhoea. Most enteric pathogens intestinal mucosa stimulate at least partial immunity against repeated • Other complications may occur, for example, infection or illness, which helps to explain the haemolytic uraemic syndrome, which may cause declining incidence of disease in older children and renal failure adults. However, some elderly adults may become • The most important cause of acute dysentery is increasingly susceptible with advancing years if they Shigella; other causes are C. The diagnosis of infective diarrhoea is dependent upon the identification of the causative pathogen Persistent diarrhoea from the faeces by culture, antigen detection or by • Begins acutely, but is of an unusually long light microscopy (in the case of parasites). In most aetiological diagnosis, although clinical features can cases the information gained by spending a few act as a rough guide. The treatment of diarrhoea minutes asking for details of the illness, and must therefore be based on the major features of observing and examining the child for specific signs the disease and an understanding of the underlying (dehydration or undernutrition) is sufficient to pathogenetic mechanisms, as described earlier. The clinical assessment should lead directly to: • a plan for treating or preventing dehydration; • a plan for treating dysentery; • a plan for treating persistent diarrhoea; • recommendations for feeding during and after diarrhoea; • a plan for managing any concurrent illness; • recommendations regarding measles immunization; and • a plan for follow-up. The top part of the chart shows how to assess Signs that are most valuable in assessing patients for dehydration and how to assess and dehydration, termed key signs, are marked with manage other important problems. Two or more circled features described in these figures are the features signs in one column, including at least one key that are most important and can be most reliably sign, means that the patient falls in that category assessed by health workers at all levels. If signs are noted in more than one column, as often Assessing the child for dehydration occurs, the category of dehydration is the one Children should first be evaluated for dehydration farthest to the right (among columns A, B, and C) and then for other problems associated with in which two items, including at least one key sign, diarrhoea. However, when a child is severely dehydrated, taking a complete history and Column C: Severe dehydration doing a thorough examination must be deferred Look first at column C. A circled in that column, including at least one key stuporous child, with severe dehydration requires sign, the patient has severe dehydration. Children with severe dehydration have a fluid The detection of dehydration is based entirely on deficit equalling more than 10% of their body clinical signs. They are usually lethargic, stuporous or identify children with diarrhoea who are at even comatose. The eyes are deeply sunken and increased risk of becoming dehydrated, for without tears; the mouth and tongue are very dry, example, those children who are vomiting, have a and breathing is rapid and deep.
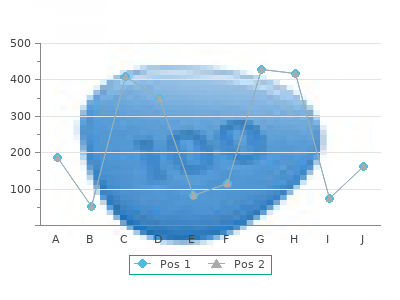
Subcutaneous hemorrhage beneath the wing of a cage- housed pullet due to Vitamin K deficiency feldene 20 mg without a prescription. Hyperkeratosis (thickening of the skin) of the plantar surface of the feet associated with pantothenic acid or biotin deficiency generic feldene 20mg otc. Fatty liver syndrome in a mature hen results in rupture and hemorrhage into the body cavity. This condition can be prevented by lowering the energy value of the feed and ensuring that sulphur- containing amino acids and choline are at an appropriate dietary inclusion rate. Generally, erosive losses of up to 20% occur in non-protected or inadequately vaccinated flocks. Marek’s disease virus is immunosuppressive and infected broiler and pullet replacement flocks are susceptible to a wide range of viral and bacterial infections. The virus is resistant to environmental exposure and can remain viable for long periods in houses especially if units are not decontaminated between cycles. Infected birds shed “dander” (feather dust) contaminated with virus which can be distributed by wind, equipment, and personnel. Death occurs in both caged and floor-housed birds as a result of dehydration and persecution. Occasionally visceral lesions are observed and the kidney, eye, proventriculus, ovary or other organs may be affected. Histological examination of nerve and visceral lesions will show characteristic 69 lymphocytic proliferation. The condition should be differentiated from botulism and from “transient paralysis”, an emerging condition of unknown etiology, but suspected to be an autoimmune response to vaccination in specific strains of commercial laying hens. The causal virus may be isolated and identified by submitting tissues to a suitably equipped laboratory using specific tissue culture techniques. Cell-associated, frozen vaccines require special storage in a liquid nitrogen canister. Careful reconstitution using the diluents supplied by the vaccine manufacturer is necessary to maintain viability of the vaccine virus. Improper vaccination technique may lead to defective immunization with resulting “breaks”. It is essential to place day old chicks in houses which have been thoroughly decontaminated to allow vaccinated flocks to develop immunity. Rearing farms and broiler growing units should be operated as single-age units with all-in-all-out cycles. Characteristic posture of an immature chicken in sternal recumbency with Marek’s disease showing alternating extension and retraction of legs. Unilateral enlargement of nerves of the sciatic plexus is characteristic of Marek’s disease. Acute infection with classic mild or variant strains results in up to 5% mortality. Avibirnaviruses are immunosuppressive and predispose flocks to intercurrent viral pathogens and secondary bacterial infection. Infectious Bursal Disease is a major restraint to productivity and profitability in the poultry industries of both industrialized and developing nations. Contaminated equipment, non-pelleted feed containing inadequately heat- treated poultry by-product meal, housing, and clothing of personnel are frequently sources of infection. Affected birds are depressed and show recumbency, ruffled plumage and white diarrhea. In acute cases the characteristic lesion comprises enlargement of the bursa of Fabricius which is often surrounded by gelatinous exudate. Histological examination of bursas from broilers or pullets at various stages of the disease will show edema progressing to atrophy. This program will promote transfer of high and uniform levels of antibodies to progeny. Broiler and replacement layer chicks should be vaccinated with live-attenuated vaccine which primes the immune system. In North America a mild live multivalent (classic and variant) vaccine is administered by the in ovo route to provide initial stimulation of the immune system. Subsequent administration of intermediate strain vaccine may be necessary depending on factors including: • Risk of infection. This formula relates the initial antibody level to the rate of decline in maternal antibody to obtain the optimal age for vaccination. It is necessary to maintain strict levels of biosecurity and to operate flocks on an all-in-all-out basis in areas where severe infectious bursal disease is endemic. Characteristic subcutaneous and intramuscular hemorrhages associated with infectious bursal disease. This condition should be differentiated from mycotoxicosis and anti-coagulant toxicity. Severe nephritis characterized by pallor and urate deposit may be associated with nephropathogenic strains of infectious bronchitis virus, infectious bursal disease or water deprivation. The virus causes stunting and increased susceptibility to secondary viral and bacterial infections including dermatitis which results in downgrading.
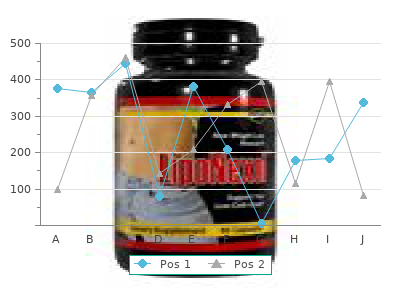
Identification—This fungal disease presents with characteristic scaling or cracking of the skin purchase feldene 20 mg with visa, especially between the toes (interdigital) purchase feldene 20mg amex, diffuse scaling over the sole of the foot (dry type) or blisters containing a thin watery fluid; commonly called athlete foot. In severe cases, vesicular lesions appear on various parts of the body, especially the hands; these dermatophytids do not contain the fungus but are an allergic reaction to fungus products. Presumptive diagnosis is verified by microscopic examination of potas- sium hydroxide-or calcofluor white-treated scrapings from lesions that reveal septate branching filaments. Note that bacteria, including Gram- negative organisms and coryneforms, as well as Candida and Scytalidium species, may produce similar lesions. They are also common in industrial workers, schoolchildren, athletes and military personnel who share shower or bathing facilities. Period of communicability—As long as lesions are present and viable spores persist on contaminated materials. Educate the public to maintain strict personal hygiene; take special care in drying between toes after bathing; regularly use a dusting powder or cream containing an effective antifungal on the feet and partic- ularly between the toes. Control of patient, contacts and the immediate environment: 1) Report to local health authority: Obligatory report of epidem- ics in some countries; no individual case report, Class 4 (see Reporting). Oral terbinafine, or itraconazole may be indicated in severe, extensive or protracted disease; griseofulvin, although less active, is an alternative. Epidemic measures: Thoroughly clean and wash floors of showers and similar sources of infection; disinfect with a fungi- cidal agent such as cresol. Identification—A chronic fungal disease involving one or more nails of the hands or feet. The nail gradually becomes detached from the nail bed, thickens, and becomes discolored and brittle, an accumulation of soft keratinous material forms beneath the nail or the nail becomes chalky and disintegrates. Diagnosis is made by microscopic examination of potassium hydroxide preparations of the nail and of detritus beneath the nail for hyaline fungal elements. Mode of transmission—Presumably through extension from skin infections acquired by direct contact with skin or nail lesions of infected people, or from indirect contact (contaminated floors and shower stalls) with a low rate of transmission, even to close family associates. Preventive measures: Cleanliness and use of a fungicidal agent such as cresol for disinfecting floors in common use; frequent hosing and rapid draining of shower rooms. Control of patient, contacts and the immediate environment: 1) Report to local health authority: Official report not ordinarily justifiable, Class 5 (see Reporting). Epidemic measures, Disaster implications and International measures: Not applicable. It is a symptom of infection by many different bacterial, viral and parasitic enteric agents. The specific diarrheal diseases—cholera, shigellosis, salmonellosis, Escherichia coli infections, yersiniosis, giardiasis, Campylobacter enteritis, cryptosporidiosis and viral gastroenteropa- thy—are each described in detail under individual listings elsewhere in this book. Diarrhea can also occur in association with other infectious diseases such as malaria and measles, as well as chemical agents. Change in the enteric flora induced by antibiotics may produce acute diarrhea by overgrowth and toxin production by Clostridium difficile. Approximately 70%–80% of the vast number of sporadic diarrheal episodes in people visiting treatment facilities in less industrialized countries could be diagnosed etiologically if the complete battery of newer laboratory tests were available and utilized. From a practical clinical standpoint, diarrheal illnesses can be divided into 3 clinical presentations: 1) Acute watery diarrhea (including cholera), lasting several hours or days; the main danger is dehydration; weight loss occurs if feeding is not continued. The details pertaining to the individual diseases are presented in separate chapters. Each has a different pathogenesis, possesses distinct virulence properties, and comprises a separate set of O:H serotypes. Transmission is usually through contaminated food, water or hands; an outbreak in 2003 in Ohio was attributed to respiratory transmission via contaminated sawdust. The diarrhea may range from mild and nonbloody to stools that are virtually all blood. Lack of fever in most patients can help to differentiate this infection from that due to other enteric pathogens. The other most common serogroups in the United States are O26, O111, O103, O45, and O121. Occurrence—These infections are an important problem in North America, Europe, Japan, the southern cone of South America and southern Africa. Mode of transmission—Mainly through ingestion of food contam- inated with ruminant feces. Direct person-to-person transmission occurs in families, child care centers and custodial institutions. Waterborne transmission occurs both from contaminated drinking water and from recreational waters. Period of communicability—The duration of excretion of the pathogen is typically 1 week or less in adults but 3 weeks in one-third of children.
